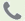ERGONOMIC GUIDELINE
DISCLAIMERThis supplement is designed to provide information which will assist employers in developing and implementing ergonomic safety policies. Necessary measures have been taken to insure the accuracy and reliability of the information contained herein, however Point of Care Consults makes no representation, warranty, or guarantee in connection therewith.
Point of Care Consults disclaims any liability or responsibility for loss or damages resulting from the use of any of the information contained herein, or for the violation of any federal, state, or local regulations with which any of the information may conflict.
Point Of Care Consults will contact purchasers by mail if new regulations are published on ergonomics within 6 months of purchase. All other notices of change will be published in our newsletter *Point of Care Consults News Update”. A complimentary copy of this publication has been enclosed with this supplement. We encourage all purchasers to subscribe. An order form is found in each issue.
Safety compliance requires a cooperative effort. Take compliance with safety seriously. If you have any questions about ergonomic safety you may call Point of Care Consults or (if applicable) your local state office for clarification. There is a nominal charge for phone assistance for regulatory information made to Point of Care Consults.
USING THE SUPPLEMENT
This supplement has been written in an easy to use question and answer format. It has been written for medical or general businesses. The white pages contain information written by the author based on text books, medical publications, medical journals and proposed regulations. Blue pages contain charts or information you will need to copy for your employees or use more than once.
Copying or reproducing any of the information on the white pages is expressly forbidden without permission from the author.
FORMAL SAFETY POLICY
__________________________________________ (name of business) has made a commitment to provide a safe working environment and believes employees have the right to know about potential health hazards associated with their work. So that employees can make knowledgeable decisions about any personal risks of employment, an ergonomic safety program has been established. This program includes policies and procedures to follow that will reduce or eliminate the potential for musculoskelital injuries.The employer accepts responsibility for employee work site safety. All employees will have access to the enclosed policies and will be encouraged to communicate all concerns and any injuries to the employer or person designated by employer to oversee safety management. Employees will follow the policies implemented by the employer. Employees will take safety training seriously and attend programs. Employees will be informed of their right to medical treatment if an injury occurs.
This supplement has been developed for the employee’s benefit and protection. All employees determined to be at risk will receive information necessary to perform their job as safely as possible.
Date Employer/ Program Administrator
_______________ __________________________________________
If administrator changes. write date and change below:
_______________ __________________________________________
_______________ __________________________________________
_______________ __________________________________________
ERGONOMICS
History:OSHA issued an ergonomics guideline on April 5,2002. A copy of this guideline is found at the end of this chapter. Although the guideline is voluntary, OSHA may inspect for compliance under the “general duty clause”. The guidelines include many questions and answers that are helpful in understanding the plan. Fill in the blanks of the following plan to personalize it to your facility..
What is ergonomics?
Ergonomics is the science of fitting jobs to the people who work in them. It is often referred to as finding a job “comfort zone”. Ergonomic injuries can affect clerical and medical staff employees. An employer should take steps to reduce or eliminate problems before they happen.
Why have an ergonomic program if there is no OSHA regulation?
Any workplace injury is reportable. OSHA requires employers to keep workplaces free from recognized hazards under the “general duty clause”. That means that even if there is no federal law that mandates ergonomic safety, it is still a workplace hazard that must be addressed. Most ergonomic injuries can easily be reduced or prevented by putting some basic safety policies in place. One workman’s compensation claim or the cost of one employee’s lost time from work is well worth the effort and nominal cost of putting safety policies in place.
Musculoskelital disorders (MSD’s) now account for more than 600,000 injuries each year serious enough to cause time off from work (general industry), each year. Health care workers report more back injuries than any other industry! Carpal tunnel syndrome (CTS) presently accounts for 65% of ALL reported occupational injury claims!
Many states have put in place ergonomic regulations at the state level. If your state has ergonomic regulations you will need to comply with the state regulations
Goal of having an ergonomic program:
The goal of having an ergonomic program is to reduce the number and severity of musculoskeletal disorders (MSD’s) caused by exposure to risk factors in the workplace’ By determining what jobs pose a risk and implementing policies and controls, the employer can reduce or eliminate on-the-job accidents and injuries. Employees will appreciate the efforts of the employer to provide a safe and healthful working environment.
Who should the program cover?
All employees performing jobs that have been determined to pose a potential risk from repetitive motions or lifting.
An ergonomic program does not cover injuries caused by slips, trips, falls or vehicle accidents
How do I determine what jobs have a risk factor?
An ergonomic program requires the employer to determine what jobs performed by the employees pose a potential risk. Use the following risk factor list as a guideline.
How do I determine what jobs have a risk factor
An ergonomic program requires the employer to determine what job as performed by the employees pose a potential risk. Use the following risk factor list as a guideline.
1. Repetition
a. Repeating the same motions every few seconds or repeating a cycle of motions more than twice per minute for more than 2 consecutive hours in a workday.
b. Using a keyboard more than 4 hours total per day.
2. Force
a. Lifting more than 75 lbs at any one time
b. Lifting more than 55 lbs more than 10 times a day
c. Pushing or pulling more than 20 lbs
3. Awkward posture
a. Working with the neck or wrists bent for more than 2 hours (total) per day
4. Vibration
a. N/A to purchasers of this publication
5. Contact stress
a. N/A to purchasers of this publication
Policy: The employer and/or safety management coordinator will determine what jobs pose a risk to employee(s) using the above guideline.
The following jobs have been determined to pose a risk to employees:
Job Risk
______________________ ______________________
______________________ ______________________
______________________ ______________________
______________________ ______________________
______________________ ______________________
What to do I do once a job risk is identified?
Once the employer/safety coordinator determines what jobs pose a risk, a job hazard analysis will be performed. The magnitude, frequency and duration of job’s exposure to risk factors will be noted. The following will be part of the job hazard analysis:
Observe the employees performing the job identified with a potential risk.
Hold a meeting that include all (or as many as possible) employee’s performing the job identified.
Talk to employees about the potential problem(s) that may lead to an ergonomic injury.
Ask employees for recommendations.
Take steps to control the ergonomic hazard or reduce it to an acceptable level.
Implement controls (work practice, engineering & PPE).
Implement policies.
Policy:The employer and/or safety management coordinator will analyze jobs that have been determined to have a risk factor. The management will investigate ways to control and/or reduce the job risk to a safe level. The management will consult with employees performing the job(s) determined to have a risk and take their concerns and recommendations into account. The management will purchase and implement controls (if applicable) and develop policies to reduce the hazard(s).
What is a Work Practice Control?
Work practice controls are changes in the way an employee performs the physical work activities of a job that can reduce or control exposure to ergonomic hazards. Work practice controls will be implemented as needed if a job hazard exists. Most work practice controls are “common sense” policies. Examples:
Neutral posture when performing a task
Taking micro breaks
Two people lift teams
Policy:The following work practice controls that have been put in place:
____________________________________________________________________________________
____________________________________________________________________________________
____________________________________________________________________________________
____________________________________________________________________________________
____________________________________________________________________________________
What is an Engineering Control?
Engineering controls are physical changes to a job that reduce job hazards. Engineering controls will be implemented as needed if a job hazard exists. Some engineering controls may also be considered personal protective equipment (e.g. back brace). Examples:
Changing or re-designing a work station
Safety equipment
Wrist pad
Wrist
brace
Back brace
ergonomic chair
Policy:The following engineering controls that have been put in place:
____________________________________________________________________________________
____________________________________________________________________________________
____________________________________________________________________________________
What if I still have a problem after implementing controls for a job hazard?
If controls and policies have been implemented and a work-relate ergonomic injury occurs, the employer/safety coordinator will:
Ensure that controls were being used
Ensure that policies were being followed
Determine if only one employee was affected or many
Determine whether new controls are needed
Policy:If controls and policies were followed and a work-relate ergonomic injury occurs, the job will be termed a “problem job”. If the analysis concludes that the risk only affected one employee - new controls may be limited to only that employee. If controls were not effective overall, the employer/safety coordinator will look for alternatives. The employer/safety management will track the progress of the new controls and/or policies implemented by consulting with employees.
What are some basic steps an employer should take?
The employer should determine what jobs pose a potential risk.
Provide each employee that perform jobs that pose risks with basic information on ergonomics. Information should contain common ergonomic injuries, their signs and symptoms, risk factors for MSD’s, the importance of reporting problems early and how to report problems.
The employer should evaluate (1) jobs that have risks (2) any reported work related ergonomic injuries and determine what policies and controls should be implemented to prevent or reduce the problem in the future.
Determine if you (the employer) will implement the policies or if you will designate the management of the ergonomic safety program to an employee. If the position is delegated, the employer must provide information and training on the regulations to the employee so they can competently take on the responsibility. Communication between the employer and safety management should be on-going.
Ask employees for input when developing policies and selecting controls.
Analyze how policies and controls are working after they have been implemented for a few months.
How extensive should my ergonomic program be?
An ergonomic program should be geared to the level of the problems you have identified. The program can be basic or a comprehensive program. Definitions of both follow.
Policy: The employer/safety management will determine how extensive the ergonomic program will be based on the following guidelines for a basic or comprehensive program. This facility has determined that a program_________________________ will be implemented.
The ergonomic program should:
Encourage employees - not discourage employees to follow policies
Encourage early reporting of ergonomic injuries
Encourage employees to participate in program
Encourage employees to communicate their concerns
Basic Program
Basic programs are often all that is needed when only minimal problems have been identified. It is often all that is needed for small businesses. Guidelines for implementing a basic programs would be:
Only a few jobs have been identified to pose a risk
No ergonomic injuries have ever been reported
Only a few isolated ergonomic injuries have ever occurred
Only one incident has occurred since putting controls and policies in place
The problem easily can be fixed
Policy: A basic program will be implemented by the employer/safety coordinator if it meets one or more of the guidelines listed above..
If the employer/safety coordinator has determined that a basic program is indicated the following will be included as part of that basic program:.
Determining what jobs pose a risk
Observing employee(s) performing job with potential risk
Talk to employee about ergonomic injuries. Discuss how they relate to the job and ask employees what controls they feel will help.
Encourage employee(s) to report problems
Providing ergonomic management to the employee(s) who report problems
Implement controls and policies
Reviewing controls and policies with employees after 30 days (recommendation) to determine if they have reduced or eliminated problem(s)
Policy: If a basic program does not reduce or eliminate the ergonomic related problem a full ergonomic program will be implemented.
Comprehensive/Full Ergonomic Program
The goal of a full ergonomic program is to reduce the number and severity of ergonomic related injuries in the workplace. It is appropriate when more than a basic program is indicated. A full ergonomic program will include:
Leadership/management of the program
Employee participation
Job risk analysis (identify and analyze problem)
Ergonomic management - hazard reduction and control
Implementing work practice and engineering controls
Providing employee training
Performing a program evaluation at least every 3 years
Look for positive results - such as a reduction in the number of MSD’s
If deficiencies are noted - correct promptly
Policy: A comprehensive/full ergonomic program will be implemented when problems indicate that more than a basic ergonomic program is needed. The employer/safety management will adjust the ergonomic program as needed to comply with federal and state laws - if applicable.
How often should I review policies?
A complete assessment of the policies and controls should be performed two or three months (recommendation) after program is implemented. If the program appears successful, future evaluations can be performed every three years (recommendation) or as needed if a problem occurs. Always document that an evaluation was performed.
Policy: The employer/safety management will re-evaluate controls and policies that have been implemented to assure they are working.
What if I already have an ergonomic program?
If the business already has an ergonomic program in place it should continue to implement the program or modify, the program based on the guidelines in this supplement. OSHA stated in the guideline that, “OSHA will not focus enforcement efforts on employers who have implemented effective ergonomic programs or who are making good-faith efforts to reduce ergonomic hazards.” If a federal standard is released, programs will need to be adjusted to comply with the federal requirements. Facilities should also check with their state (local) OSHA and department of labor to see if their state has passed any ergonomic regulations for businesses.
Policy: The employer/safety management will adjust the ergonomic program as needed to comply with federal and state laws (if applicable).
UNDERSTANDING MUSCULOSKELITAL DISORDERS (MSD,S)
What is a Musculoskelital Disorder?A MSD is a disorder that can affect muscles, nerves, tendons, ligament, joints, cartilage, blood kessels or spinal disks. This can include muscle strains and tears, ligament sprains, joint and tendon inflammation, pinched nerves and spinal disc degeneration. This supplement uses the term musculoskelital disorders (MSD’s) to describe ergonomic related injuries, however, other publications may use terms such as repetitive stress injuries (RSI’s) and cumulative trauma disorders (CTD’s).
What areas of the body are commonly effected by MSD’s?
MSD’s can effect many areas of the body depending on the job task performed. Common problem areas include:
Neck
Shoulder
Back
Knee
Ankle
Foot
Wrist
Hand
Elbow
Forearm
Abdomen (hernia only)
What are the common causes of MSD’s?
Common causes that can result in an MSD include:
Awkward posture
Repetitive motion
Improper lifting
Contact stress
Extreme force
Vibration
MSD Medical conditions include:
Lower back pain
Tension neck syndrome
Carpal tunnel syndrome
Rotator cuff syndrome
Sciatica
Tendinitis
DeQuevain’s syndrome
Trigger finger
Tarsal tunnel syndrome
Herniated spinal disc
Thoracic Outlet Syndrome
What are the Signs and Symptoms of a MSD?
Common signs on a MSD may include decreased range of motion, decreased grip strength, loss of muscle function and deformity. Symptoms of an MSD may include pain, numbness, tingling, burning, cramping and stiffness. A MSD with a symptom of only slight discomfort would not (in most cases) be covered by the program.
How common are MSD’s?
Common signs on a MSD may include decreased range of motion, decreased grip strength, loss of muscle function and deformity. Symptoms of an MSD may include pain, numbness, tingling, burning, cramping and stiffness. A MSD with a symptom of only slight discomfort would not (in most cases) be covered by the program.
How common are MSD’s?
Carpal tunnel syndrome (CTS) presently account for 65% of All reported occupational injuries reported! Back injuries account for the highest amount of injuries reported among health care workers. Back injuries are a problem in many other jobs as well.
What is a MSD Incident
A MSD incident is a work related MSD that requires the employee to:
miss days from work
need to have their job modified or restricted due to injury
seek medical treatment beyond first aid
when employee reports that signs or symptoms of an MSD has lasted for more than 7 consecutive days
Policy: If a MSD incident occurs the employer/safety manager will provide the employee with medical consultation and treatment (if indicated). Steps will be take to correct the problem from recurring
FIVE COMMON MSD’S
The following section contains more detailed information on some of the more common MSD’s experienced by people working in medical facilities. Never self-diagnose - always see a medical specialist for diagnosis. Jobs in medical facilities that can lead to these problems have been used as examples but they are not the only jobs that can result in these problems.Carpal Tunnel Syndrome (CTS)
CTS occurs when there is pressure on the nerve where it goes through the carpal tunnel. Repetitive motion of the hand or wrist may cause the tendons to become inflamed and press the nerve against the bone. The result is pain, numbness, or tingling in one or both hands. The most common cause is prolonged computer use. If symptoms are experienced, the first rule is not to ignore them. If untreated, the disorder can cause permanent nerve damage. It is important to see a specialist to confirm diagnosis. To treat the problem, stop the activity that is triggering the problem. If the symptoms decrease, introduce the activity gradually, taking care to keep the wrist straight. Never spend more than two hours doing the activity. Do exercises to wann the hands and increase circulation. Place the keyboard at a level where the wrist will be straight. Use aspirin, ibuprofen or acetaminophen to relieve pain. Apply ice packs to the palm side of the wrist. Use a wrist splint (available at pharmacies). Wear the splint when sleeping. Reduce the amount of salt in your diet - salt can increase water retention and add to swelling.
Tendinitis
A tendon is a band of tough, white, fibrous tissue that connects muscle to the bone. Muscle fibers merge into one end of a tendon, while the opposite end is attached to the bone. The tendon conveys the action of muscles to bone. Most tendons are encased in a sheath of membrane that secretes a lubricating fluid for easy sliding. Both tendons and their sheaths are vulnerable to injury and inflammation from overexertion, tearing, stretching, twisting and other trauma. Tendinitis is a disorder that causes swelling, soreness and impaired motion of the tendon. If the problem involves both the sheath and the tendon, it is tenosynovitis. To treat the problem, resting the joint, soaking in hot water to reduce swelling and taking aspirin, prescription non-steroidal anti-inflammatory drugs or other analgesics for pain are helpful. The physician may inject a steroid preparation at the site of tenderness, which should help provide relief. When pain subsides, carefully supervised range-of motion exercises should begin.
DeQuervain’s Tendinitis
Tendinitis is common in phlebotomists who draw blood all day and lab technicians that sit at a microscope for prolonged periods. Two tendons involved in pulling the thumb out and back from the hand are affected by this disorder. These tendons run in a tunnel on the side of the wrist just above the thumb. The inflammation of the tendons from overuse can eventually result in the formation of thick, bumpy and irregular tissue. The first symptom may be soreness on the thumb side of the forearm. The pain can spread up the forearm or down into the wrist and thumb if not treated. Therefore, it is imperative to see a specialist and have the condition diagnosed. To prevent the problem take frequent breaks or limit the time performing the task. Keep the wrist in a neutral alignment by wearing a brace. Take anti-inflammatory medications such as aspirin, ibuprofen or naprosyn. If anti-inflammatory medication does not help - a cortisone injection may help. If all fails, surgery may be recommended.
Lower Back Pain
Back pain afflicts four out of five Americans at one time or another. In most cases, the disability arises from weakness of the musculature surrounding the spine. Only 15% of lower back pain cases are traceable to structural defects, such as ruptured disc, arthritis or tumors. Therefore, the most important element of treatment for back pain involves strengthening and protecting supporting muscles and maintaining correct posture. The spinal column is made up of 33 bone segments (vertebrae), held together with tough bands of tissue called ligaments. Nerve roots pass through openings between the vertebrae. Thus, a severe wrench of the back or a failure of muscular support may result in the painful “pinching” of a nerve. The sciatic nerve is particularly vulnerable to such pressure. Back pain leading to the deterioration of the muscles supporting the spine can be traced to numerous conditions, therefore a physician should evaluate and diagnose any back pain before treatment is recommended. Treatment will depend on the condition. Treatment may include rest, medication, weight reduction, correcting posture and exercises (after acute pain subsides).
Thoracic Outlet Syndrom (TOS)
Problems can occur when a lab tech has poor posture or positioning when working in front of a instrument. The condition affects the shoulder, arm and hand. The cause is compression of the nerves and arteries of the arm in the thoracic outlet. An example of the activity is one that requires the arms to be extended forward - such as sitting in front of a laboratory instrument. Slouching forward and dropping the shoulders is the likely cause. This results in tendons and muscles at the side of the neck and constriction of the arteries and nerves. Symptoms are pain, weakness, numbness and tingling, swelling, fatigue or coldness in the arm and hand. TOS is hard to diagnose since it mimics other conditions such as a herniated disk in the neck or bursitis in the shoulder. To prevent or treat the condition, maintain good posture and overall conditioning. Limit the length of time that arms are outstretched. Avoid bending the neck back for long periods of time. Avoid stress and exercise to loosen up tight muscles and joints. Modification of work activities is the best management. Surgery is the last resort. Reference: Caskey, Cheryl. Ergonomics in the Clinical Laboratory. Clinical Laboratory Medicine, May/June 1999.
ERGONOMIC POLICIES FOR
COMPUTER SAFETY
The extent of the ergonomic policies needed will be based on the job risk analysis. The following checklist can help determine potential problems.COMPUTER SAFETY
Policy: The employer/safety management will evaluate computer use and put in place computer safety policies as indicated by the job risk analysis.
Use the following check list to analyze safe computer use.
Work station – Desk
Is there enough space to accommodate comfortably all equipment and materials (books/papers)?
If space is small is there a place where items not being used can be stored?
Is there enough leg-room under the desk? (3 - 6 “ from the top of the thigh to the desk is acceptable)
Is there enough space under the desk for legs and feet to get close enough to desk?
Chair
Does the chair have adjustable height?
Does the chair have an adjustable back?
Does the chair have a 5 star base (legs)?
Does the chair have a backrest that provides support for lower back?
Does the chair’s seat width and depth accommodates the size of the employee?
Does the chair seat have a “waterfall” front?
Does the chair have armrest that support both forearm
If the front edge of chair about 5" from the back of the knee?
Keyboard
Is the keyboard positioned directly in front of the operator?
Is the keyboard level 3-4" lower than the average writing surface?
Does the level of the keyboard allow straight/parallel hand-forearm posture?
Is the platform stable?
Can the mouse can be operated without reaching?
Is the keyboard elevated about 2" in rear or slope no greater than 15'?
Are elbows bent at a 90' angle when operator sits at keyboard?
Do wrists do not rest on hard edge? (not acceptable !)
Monitor
Is monitor directly in front of employee? (recommended: 18 - 29" from eyes) Is the top line of screen at or slightly below eye level? (head should tilt 15° or less)
Is the distance from operator 18-29" from the eyes? Can employees with bifocals can read screen without bending head or neck backward? (employees with bi or trifocals should be encouraged to get a “computer distance” prescription that will prevent this problem)
Does the distance from the monitor allows the employee to read screen without leaning forward or backward?
Is the screen print brighter than the screen background?
If glare from windows or lights hit the screen have steps been taken to reduce glare on the screen? This can be accomplished by; close the blinds or curtains, not have the screen facing a window, using an anti-glare screen, putting the monitor “in between” overhead lights.
Posture (picture provided on next page)
Do wrist should extend straight out from forearm (90°)
Are elbows bent at 90°?
Does employee sit with back straight and lower back supported?
Is chair adjusted so that feet can be flat on the floor? Feet should never dangle. If feet do not reach floor use a foot rest or platform.
Are knees as high as the employees hips (90°)?
Do thighs have clearance space (3-5") between chair and desk?
Reducing Problems
Proper arrangement of the work station is only part of the battle to prevent MSD’s. There are many simple ways to reduce problems. The following accessories can help prevent problems.
Accessories:
Document holder: stable and large enough to hold document/book etc.
Wrist rests: padded with no square edges. Allows employee to keep forearms, wrists and hands straight and parallel.
Wrist supports (available at most drug stores or office supply stores)
Telephone accessories such as a head set or phone receiver support that allow neck to remain straight when cradling phone on shoulder.
Light source should not cause a glare on the screen.
Mouse should be operated without reaching
COMPUTER USER EXERCISES
Exercises will help to reduce muscle stress and fatigue. Studies have suggested a 3-5 minute break every hour to prevent fatigue, stiffness and potential MSD’s. Most exercises can be performed right at their desk. Teaching these exercises should be part of the safety education program. Employees should have the approval of their family practice physician before starting any exercise program. Try each of these exercises 3 - 5 times.Neck & Head Exercises
(1) With head in natural position, tilt head and neck to left shoulder, keeping shoulder lowered. Then repeat - tilting to the right.
(2) While sitting or standing, bend head until chin is touching chest. Keeping Shoulders lowered, turn face to left side and then to right.
(3) While sitting or standing, breathe deeply and slowly touch chin to chest while exhaling. Hold briefly and tip head as far back as possible while slowly inhaling.
Back & shoulder exercises
(1) While sitting or standing, clasp hands together above the head. Stretch arms up while pushing shoulder blades together and inhaling slowly. Hold briefly and slowly lower hands to head while exhaling.
(2) From a sitting position, slowly bend your upper body down toward your knees. Hold for a few seconds - then sit up and relax.
(3) Sit in a chair with arms hanging comfortably at the sides. Inhale slowly while raising the shoulders up and backwards, keeping head tucked in. Hold for 5 seconds and slowly return to the original position while exhaling
(4) Interlace fingers then straighten arms out in front of you. Palms facing away. Hold 10 seconds.
Arm exercises
(1) Raise arms out to sides keeping elbows straight. Make small circles with your hands, 5 forward and 5 backward.
(2) Fold your arms at shoulder height then push your elbows back and hold the position for a few seconds.
(3) Roll your shoulders forward, then roll your shoulders backward.
Wrist exercises
(1) Extend your arms out in front of you -palms down. Bend wrist up - hold 10 seconds then bend your wrist down - hold i0 seconds. Stretch forearm muscles while doing this exercise.
(2) Make a tight fist and hold for a few seconds. Spread your fingers apart as widely as possible and hold for 5 seconds.
Leg exercises
(1) Grasp one shin and slowly pull your knee toward your chest. Hold for 5 seconds, then do the same for the other leg.
(2) While standing or seated or with your feet on a footrest, raise your heels up, resting the balls of your feet, so the calf muscles are flexed. Hold for a few seconds.
Eye Fatigue and Eye Exercises
Eye fatigue is a common problem with computer users. Eye fatigue is often termed “computer vision syndrome”. The following are some tips to avoid eye fatigue:
Eyeglass wearer should keep screen a little lower than eye level
Eyeglass wearer may need to get a prescription for correction at computer screen distance
Consider tinted glasses to minimize glare
Place document being copied at screen level
Do not “stare” at screen
Do not sit and stare at the computer for long periods of time
Use “new” eye drops, such as “Visine Teats” to sooth eyes
Reduce intense color contrasts between the background and the printed text
Eye Exercises
1. Palming - place the palms of the hands over the eyes and gently massage in small circles
2. Form shallow cups with the palms of your hands. Place them lightly over closed eyes - lower parts of palms on cheeks and fingers on forehead.
3. Focus change - take a break and look at objects (i.e. out a window) at a distance different from that of the computer screen.
4. Deep wink. Wink each eye separately. Blink frequently.
5. Close eyelids very tightly for 5-7 seconds, then open them wide
6. Roll eyes clockwise then counter clockwise
ERGONOMIC POLICIES FOR BACK SAFETY
Back injuries are the #1 workplace safety problem in the U.S. Anyone who’s job requires heavy lifting or moving arc at risk. Nurses and nurses aids have the highest reported back injury rate of any U. S employee! Back injuries cost an average of $8,000 - $10,000 per case. OSHA knows that most back injuries are preventable. Employers can reduce back injuries with work practice controls, engineering controls, PPE and safety training. OSHA fact: Every pound lifted puts about 7.5 lbs of pressure on the back!Policy: The employer/safety management will put in place back safety policies as indicated by the job risk analysis of jobs being performed. Employees will follow lifting policies, report any back injuries to the employer/safety management and take safety training programs when offered.
Work Practice Controls Work practice controls are “common sense”. The following are “general” work practice controls that can reduce or eliminate potential injuries:
Think before you lift - plan your move
Check object you a.re lifting for (1) secure handles (2) sharp edges (3) slippery or wet areas
Check pathway of lift
Keep weight to be lifted as light as possible
Ask for help!
If 2 people are doing move - communicate move before lifting
Face the load
Keep footing secure - about 6-12 inches apart
Bend at your knees not at your waist
Do not twist while lifting
If you need to turn - pivot entire body
Grasp object firmly
Before you lift, tuck your pelvis under and firm up your stomach muscles
Lift with your leg muscles
Keep the object close to your body
Take your time
Keep your head up and back aligned
Do not jerk the object
If you are losing grip - set object down and start again
If you need to lift an object above your waist - set it down at the half way point – then continue
Push - don’t pull - if possible
Don’t lean forward
Stay close to load
Use both arms
Engineering controls and Personal Protective Equipment
Engineering controls are physical changes or equipment made available by the employer to reduce on the job injuries. Personal protective equipment is something the employer can wear to reduce an injury. The following are some “general” engineering controls and personal protective equipment that may be indicated after analyzing back injury risks.
Use a hand truck, dolly or cart if object is very heavy or an awkward size
Wear a back brace
Use gloves to protect hands - if applicable
What Employees Can Do to Reduce Injuries
The employer/safety management can help reduce injuries through implementing work practice controls, engineering controls, personal protective equipment and offering back safety training. However, the employee can also help prevent back injuries by keeping in “good physical condition”. As with any exercise program - the employee should consult a physician if there is any question about performing any exercise. The following are some suggestions:
Keep body weight near the ideal
Practice good posture
Exercise regularly to keep your back toned and flexible
Know your capabilities and don’t exceed them
Ask for help!
The following page contains back exercises employees can do at home. Exercise programs should only be started after the approval of the employee’s physician.
BACK EXERCISES
Exercises that strengthen the stomach and back muscles will help prevent injuries. The following are some easy to perform exercises the employees can do at home.Knee to Shoulder
Lie on your back with your knees bent, feet flat on the floor and arms at your sides. Grasp your right knee and gently pull it up toward your right shoulder. Return to the starting position and repeat with the left leg
Trunk Flexion
Sitting near the edge of a chair, spread your legs and cross your arms over your chest. Tuck your chin and slowly curl your trunk downward. Relax. Uncurl slowly into an upright position, raising your head last. Be sure chair will not slip!
Press Up’s - Back Extensions
Lie on your stomach with your hands in position as if preparing for a push-up. Slowly lift your torso while keeping your hips and legs down in contact with the floor. Raise your torso, slowly increasing the lower back curve to a point where you feel a stretch, then lower yourself back down to the starting position. Repeat
Partial sit-ups
Lie on your back with your knees bent and feet flat on the floor. Tighten your stomach muscles, press your lower back to the floor. Tuck your chin into your chest and slowly curl your upper body off the floor, while reaching with your arms between your knees. Return to start position and relax your stomach and lower back
Tips: Start with a few and work number up slowly. To increase difficulty, fold your arms across your chest or grasp your hands behind your head (not neck)
Wall slide
Stand with your back pressed against a wall, and your feet about 12 inches in front of you. Slide down the wall until your hips and knees are bent at a 45-60° angle. Slowly slide back up.
Walking and swimming are an excellent exercises that are easy on the back.
Back Exercise Tips
Never force a stretch
Always stretch gently and stop if you have pain
Always start with a few repetitions and work up
If in doubt - consult your doctor before starting any exercises
BACK INJURIES COMMON IN THE MEDICAL PROFESSION
The medical profession has it’s own unique back problems stemming from moving patients. Lifting a patient can be just as strenuous and dangerous as lifting a non-breathing object, however one advantage is that you can communicate the move (in most cases) to a patient and a patient is more flexible than a box!Communication is the key to a safe move. Check the patient’s chart and determine the patient’s condition, size as well as any physical, visual, hearing, or mental impairments.
If the patient can understand, ask what they can do such as; (1) pull themselves up (2) help with hands or legs. Communicate how you plan to do the move to patient or anyone helping you
The following are some common patient transfer and safety guidelines on how to prevent or reduce the risk.
Pulling Up a Patient in Bed
1. If patient can help
a. Reach under the patient’s shoulders and waist
b. Keep your feet wide apart, knees bent and toes pointed in the direction you’ll move the patient
c. On signal, slide the patient as he pushes up with his feet until he is at top of bed
2. If patient is helpless
a. Get an assistant
b. Put a plastic bag or liner under the sheet to make sliding easier
c. Make sure you and your assistant grab same sheet and move (slide) the patient up
Patient Transfer - Bed or Exam Table to Wheelchair
(1) If possible - adjust bed or table height to waist level
(2) Lock brakes on wheelchair
(3) Make sure patient has non-slip footwear
(4) Move the patient to edge of the bed, moving first then head and shoulders, then the buttocks, then the legs and feet. Raising the head of bed (side rails up) or exam table will help.
(5) If you use a transfer belt - put it around patients waist and lift grabbing belt. If you don’t use a belt analyze how you can safely grasp the patient (i.e. hold under arms).
(6) Brace your knees against the patient’s knees
(7) Make sure the patients feet are firmly planted
(8) Keep your knees and hips flexed
(9) Get in close to the patient and hold onto belt or grasp under arms
(10) On signal, move the patient to a standing position. Straighten out your knees.
(11) With patient standing, pivot, taking little steps and staying close to the patient
(12) Don’t twist
(13) Keep your knees slightly bent, your head up, back aligned and stomach muscles contracted
(14) Lower the patient into the wheelchair by bending your knees
(15) Patient may hold onto your waist or shoulders - not your neck Reverse for wheel chair to table/bed
Bed-to-Gurney Transfer
(1) If patient is too sick or unable to help - get an assistant
(2) Adjust the bed to the level or the gurney - lock the brakes on both
(3) Move the patient to the edge of the bed
(4) Standing beside you assistant, face the patient and each place one of your knees on the gurney.
(5) Contract your stomach muscles and pull on the draw sheet on the count of three
(6) Move the patient first to the edge and then to the middle of the gurney
(7) Keep your head up and your back aligned
(8) Keep movement smooth - don’t jerk. Reverse the process when transferring from gurney to bed
Patient moving tips
If patient is too large and unable to assist you - get help
Moving a patient by yourself should be the last resort
Use common sense (work practice controls) and engineering controls (i.e. mechanical lifting device) if available
Employee(s) must be instructed on use of a mechanical lifting device.
If the patient starts to fall;
(1) Don’t try to stop fall
(2) Grasp patient and get as close as you can to guide patient to the floor
(3) Bend your hips, not your back
(4) Get help to get patient off the floor
ERGONOMIC INJURY MANAGEMENT & RECORD KEEPING
Policy: All reported ergonomic injuries will be given prompt attention. Employees will be made aware of the importance of reporting potential ergonomic injuries when symptoms occur. Employees will be aware of (1) who to report the problem to (2) the policies for reporting ergonomic injuries, and (3) the management and follow-up after reporting the ergonomic injury.What should the employer do if an employee reports an ergonomic related injury?
Promptly determine whether the problem qualifies as an ergonomic related injury or MSD. Next it must be determined if the MSD work related. The screening questions below and their answers will help determine how serious the problem is. The help of a health care professional (HCP) may be needed.
Did the MSD require the employee to take days off from work or have work restricted?
Did the MSD require medical treatment beyond first aid?
Did the signs and symptoms last for 7 consecutive days?
If the answer is “yes” to these questions, the employer/safety management will document the problem and take steps to correct it. If the answer is “no” - no further action is required.
Management of Ergonomic Injuries
The employer/safety management will provide the employee with prompt medical management if the ergonomic injury is determined to be work related. All medical management is at no cost to the employee.
This management will include:
Referral to a HCP for injury assessment and treatment
Work restrictions or time off - if recommended by the HCP while recovering.
Evaluation and follow up of the incident
HCP Injury Assessment
The employer/safety management will provide the HCP who will evaluate the injury with the following information:
Description of employee’s job
Physical work activities
Job risk factor
When problem was reported
HCP Written Opinion
The employer/safety management will obtain a written opinion from the HCP for each assessment conducted. The written opinion will not include any findings not related to the injury. The opinion will be promptly reviewed and act upon. The written opinion from the HCP who has evaluated the employee’s injury will include the following information:
Assessment of physical condition as it related to job
Recommendations for work restrictions (if applicable)
Recommendations for time off to recover (if applicable)
Follow-up needed (i.e. physical therapy)
A statement that employee has been informed of results of evaluation and follow-up
A statement that employee has been informed about activities that could impede recovery
Work Restrictions
If the HCP assessment indicates the employee needs work restrictions or time off from work - the employer will provide what has been recommended. If recommended a temporary job alternatives will be offered. The employee will be provided with “work restriction protection”. Work restriction protection includes benefits and wages until:
1. Employee is able to resume job without hindering recovery
2. HCP determines employee can never resume job
What if the employee wants a second opinion?
A employee may consult their own HCP - at no cost to them - if they request a second opinion. If the second opinion does not agree with the first opinion - the two HCP are to consult and discuss and resolve the disagreement. If the problem is not resolved - a 3rd opinion may be obtained.
Management Record Keeping of Ergonomic Injuries
The employer/safety manager will keep written records of the following:Employee reports of ergonomic related injuries
Response to such reports
Review of the job hazard and problem
HCP consultation
Work restrictions
Record of workers’ compensation
Job hazard analysis
How problem has been corrected
HCP opinion
Insurance company reports
OSHA 300 Log
As on January 1, 2002 OSHA 200/300 illness and injury forms are no longer required for medical and dental facilities. Facilities must keep incident reports and keep follow up records for job related injuries. If a business is not exempt for OSHA 200/300 record keeping - the injury will be recorded in accordance with OSHA record keeping regulations. OSHA 300 logs and instructions are available on OSHA web site or may be obtained from your local OSHA office.
Ergonomic Record Retention
The employer/safety management will retain all ergonomic injury records in accordance with the OSHA regulations for on-the-job injuries and illnesses.
HCP opinions of injuries are to be retained for the duration of the employees employment plus 3 years. If the employee has worked less than 1 year, you may provide the employee with the record of their injury upon their leaving the employment.
If applicable - keep OSHA 300 logs for 5 years
ERGONOMIC SAFETY TRAINING
Policy for employees: Ergonomic safety training will be provided within 14 days (recommended) of hire to any employee who will perform a job that has been identified to pose a risk. Initial training upon hire is not required if employee has had documented training for same job within past 3 years. The training will be given in language employee can understand. After the initial training, training will reviewed at least every three years (recommended).Policy for safety coordinator: The employer must provide information and training to the safety coordinator and/or management on the standard so that the safety management can effectively and intelligently implement the safety training program.
Training will include:
Description of the ergonomic program
Basic information about common ergonomic injuries (ones that apply to the employee’s job)
Signs and symptoms of ergonomic injuries (ones that apply to the employee’s job)
How to identify the risk factors
Potential hazards
Controls (work practice, engineering, personal protection) to be used
How to report injuries
Training Aids
Training booklets have been provided with this supplement. There is a sample quiz found at the end of each booklet. It is not mandatory that you give a quiz, however, it can serve as good documentation of the session. Last, a certificate to document training follows this page.
REFERENCES USED IN THIS SUPPLEMENT
ISHN December 2000, OSHA’s Ergonomic Standard Covers 6.1 Million Work Sites Job Safety and Health Quarterly Fitting the Job to the Worker Washington Report December 7, 2000, OSHA Issues New Ergonomics Rule Caskey, Cheryl. Ergonomics in the Clinical Laboratory. Clinical Laboratory Medicine. May/June 2000.Giles, Terry The Body Friendly Workstation (pamphlet)
Costal Safety and Environmental Health Booklets
Office Safety. 2000
Office Ergonomics. 1998
Video Display Terminals 1999
Protecting Your Back. 1996
Federal Register November 14, 2000, OSHA 29 CRF 1910, Ergonomics Program Final Rule
OSHA National News Release April 5, 2002, Comprehensive Plan to Reduce Ergonomic Injuries.
 Hours:
Hours: